Success Rates
We’re passionate about helping patients achieve their dream of having a family. It’s a responsibility we take very seriously. We believe in empowering you with relevant information so you can make the best decisions for your individual circumstances.
That’s why we believe in complete transparency when it comes to publishing our IVF pregnancy success rates.
Understanding IVF success rates
We understand that interpreting success rates and comparing fertility clinics can be challenging, as different providers often present their success rates in very different ways. It’s important to us that you’re able to make an informed decision when choosing a fertility provider. You can access independent guidance and information on how to interpret success rates by clicking here.
On this page, you will find two different representations of success rates; YourIVFSuccess and ANZARD Success Rates. Each of these representations use unique sets of data in order to explain the key measures of success of different treatments. Be sure to read through the information carefully and contact our nurse enquiry team should you have any questions.
YourIVFSuccess Rates
YourIVFSuccess is independently published data by the University of New South Wales and shows the success rates of each clinic around Australia compared to the national average. The publication of this data is voluntary.
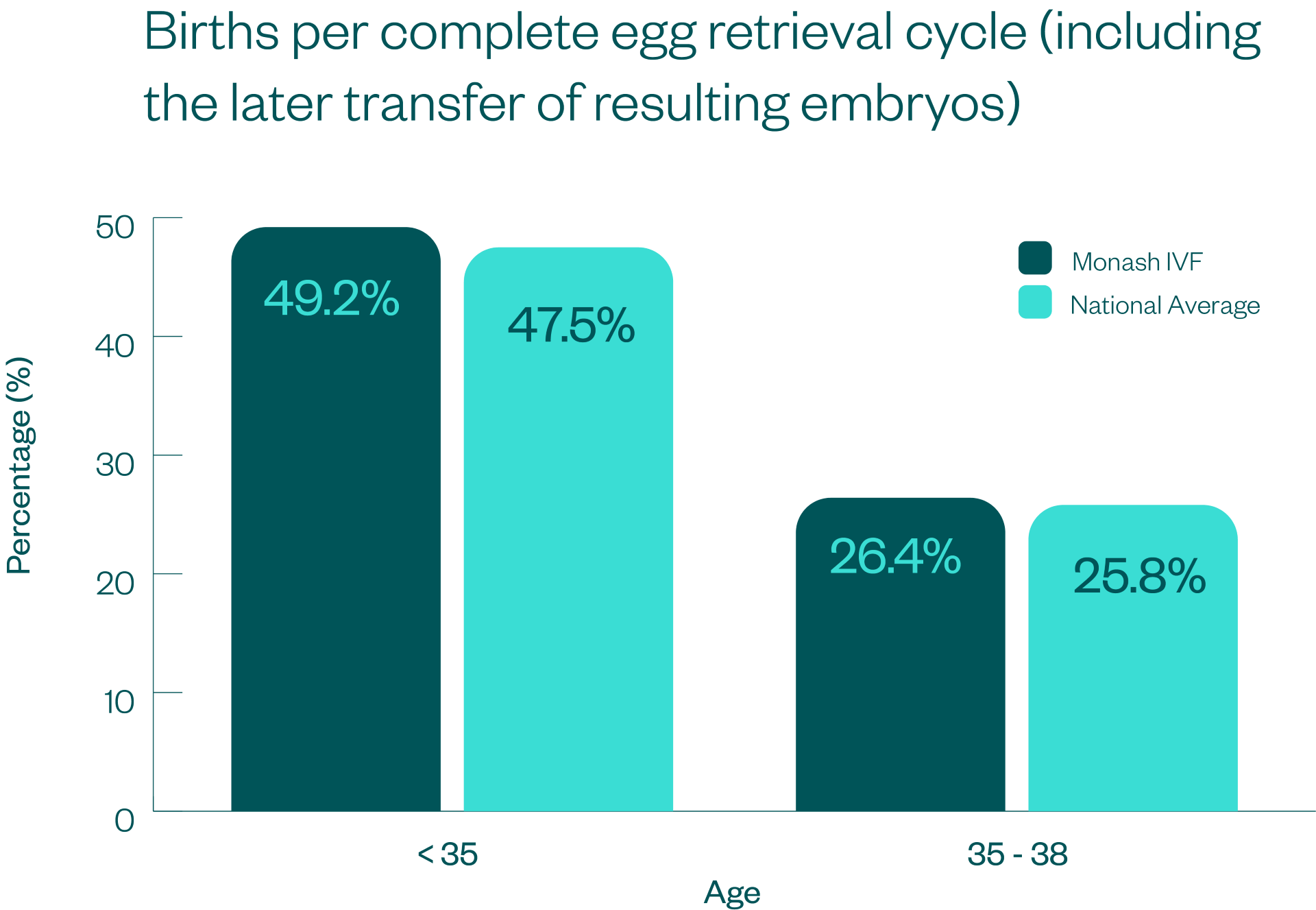
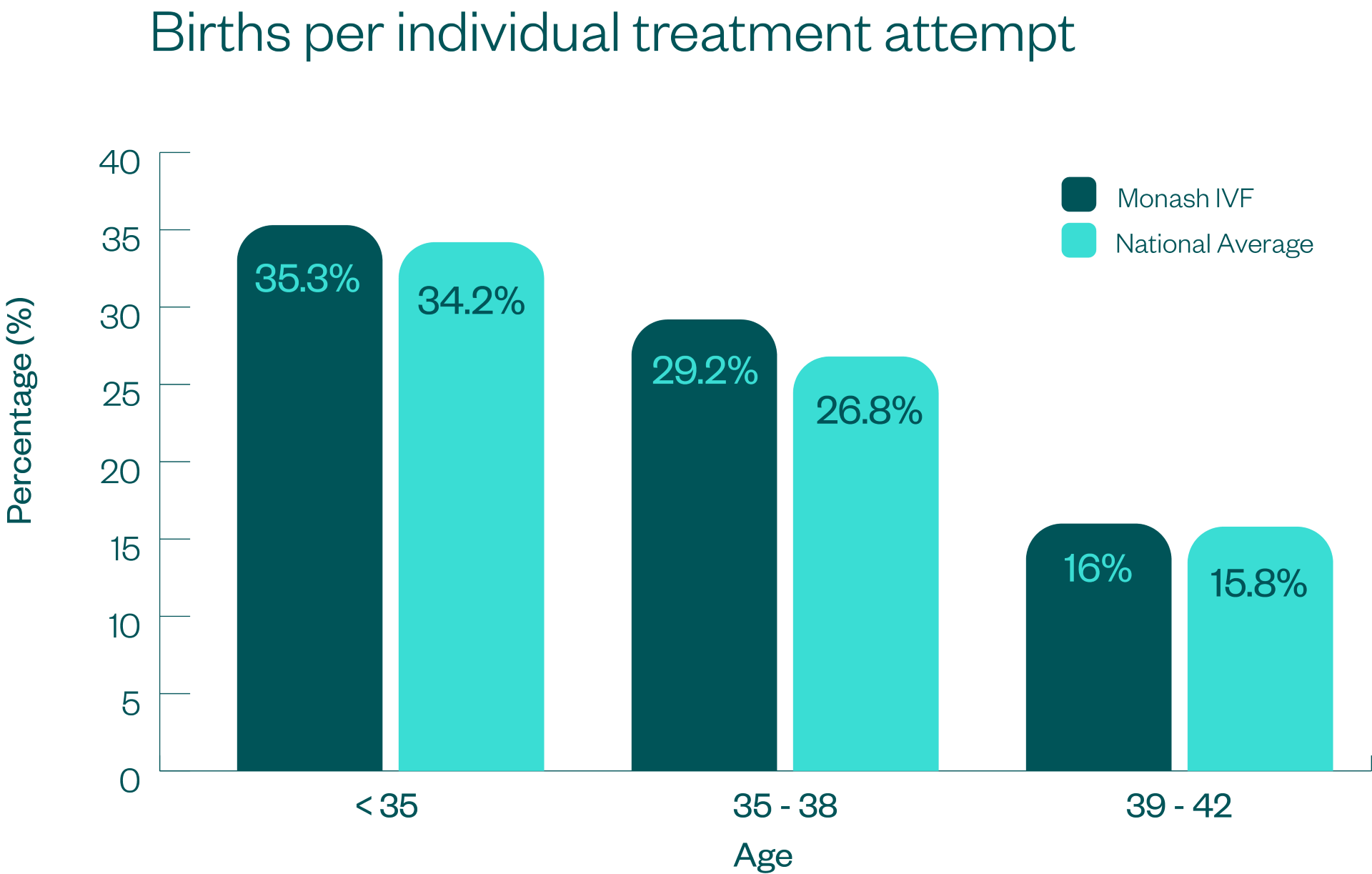
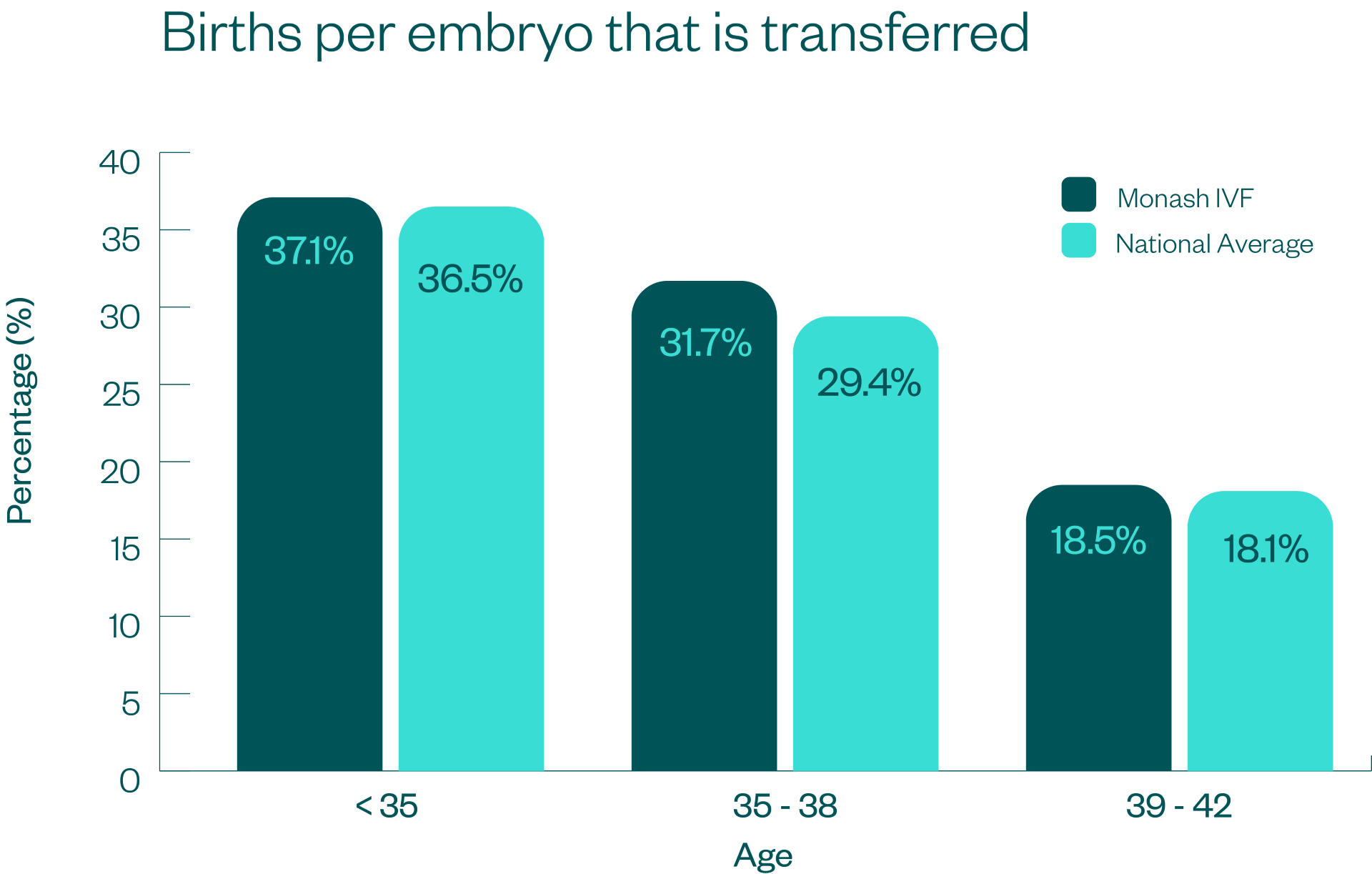
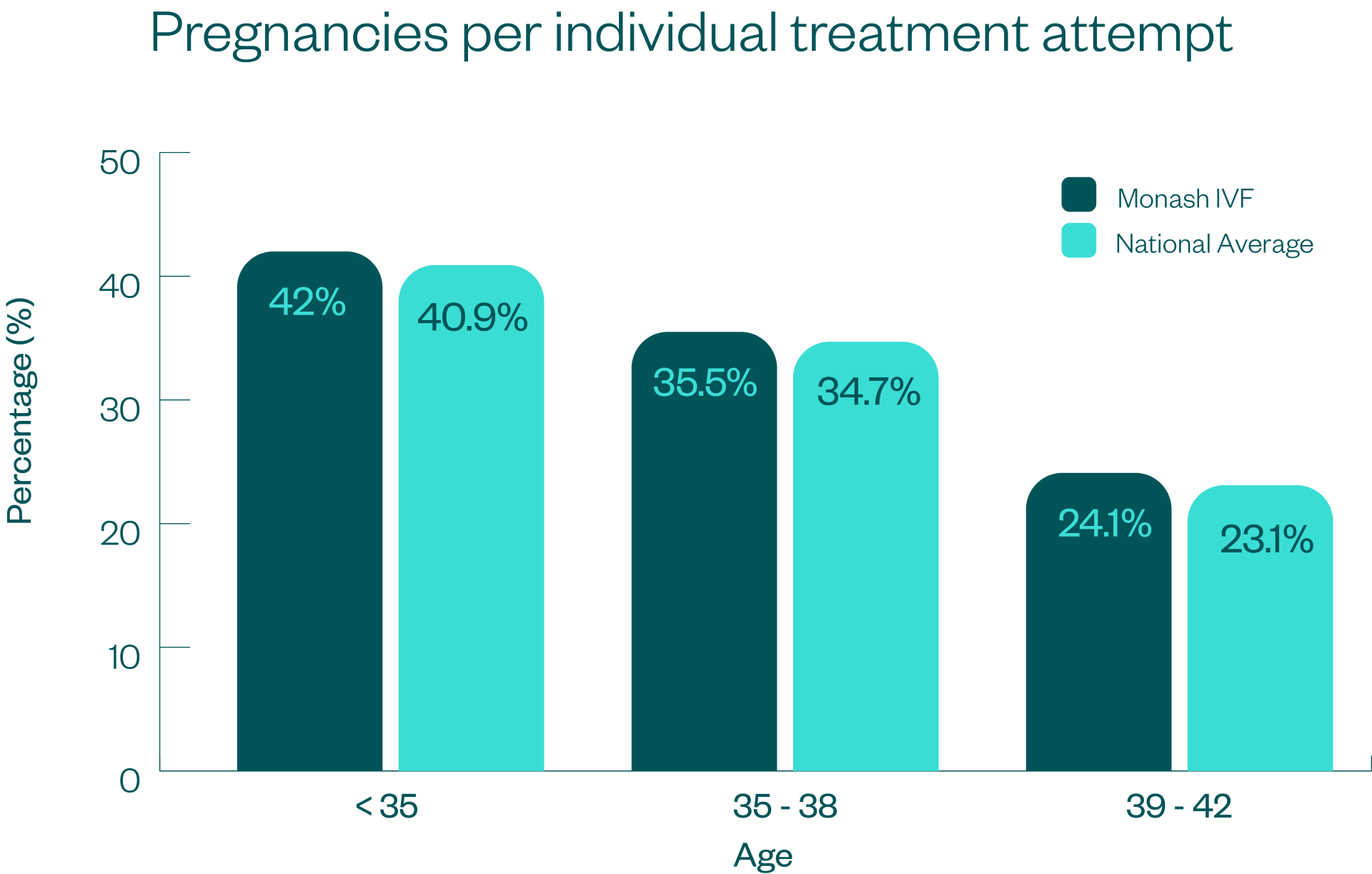
This data is presented using 5 key measures which are demonstrated in the graphs below, along with an explanation of what the measure means, and how it is calculated.
ANZARD Success Rates Results
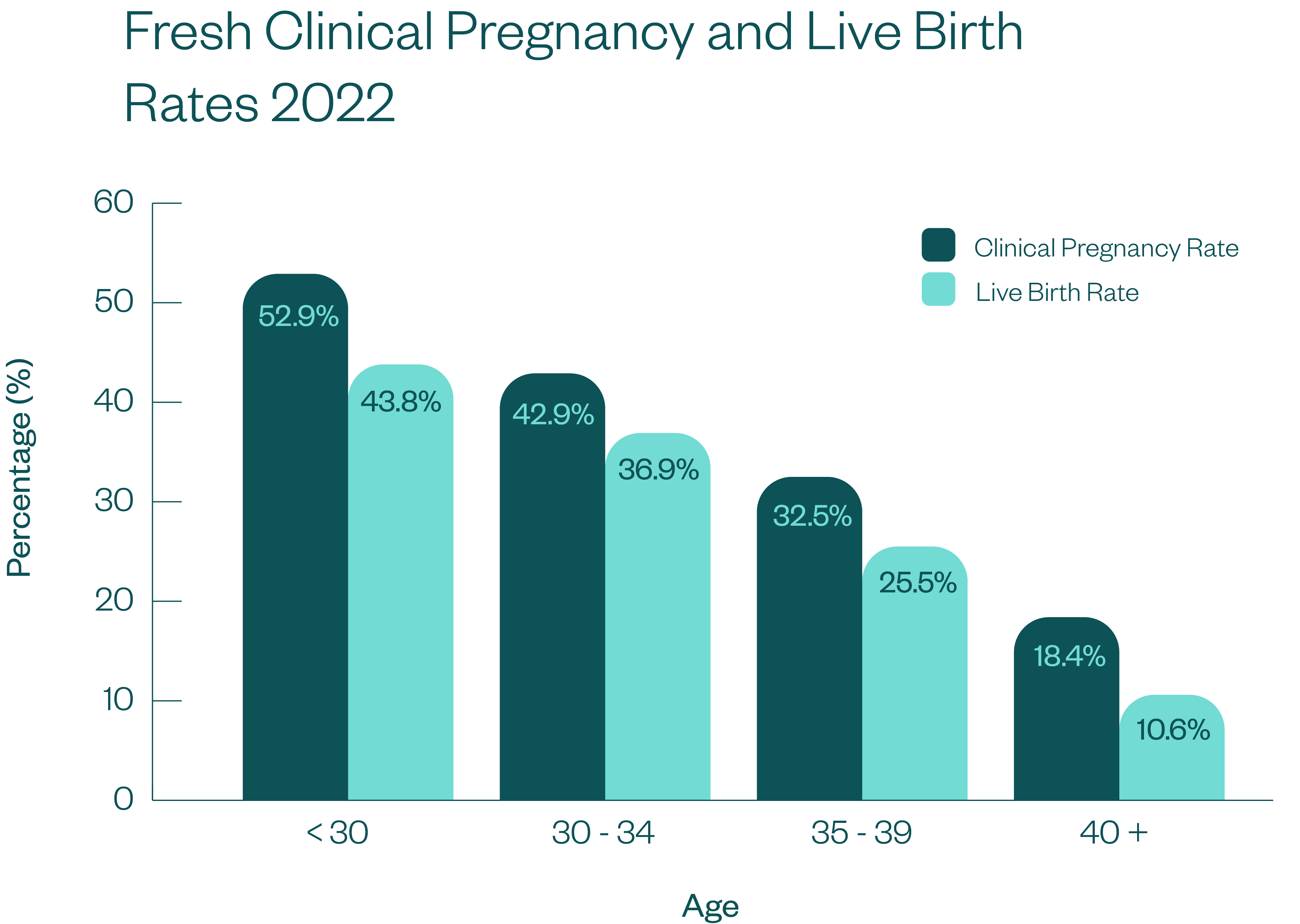
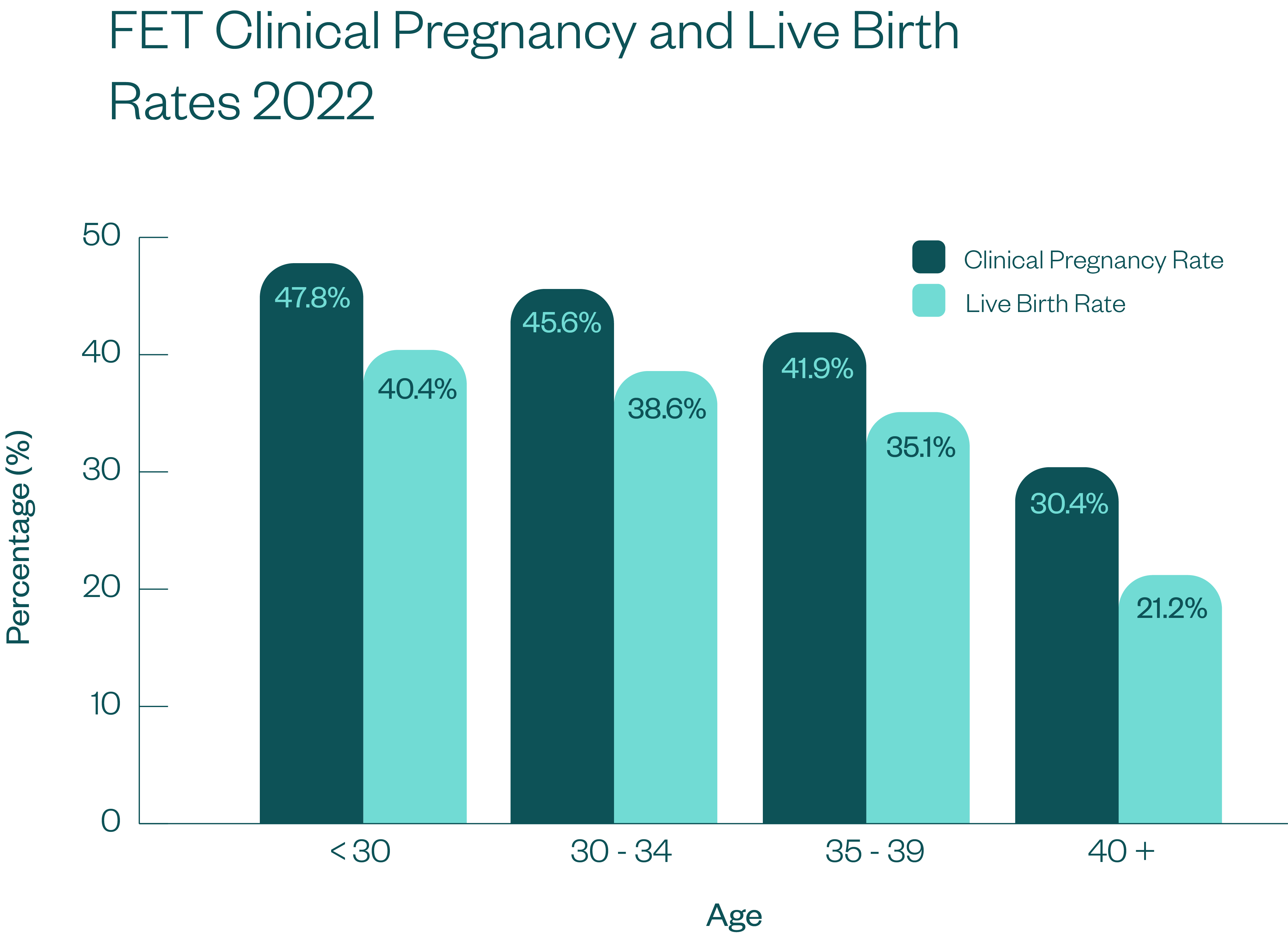
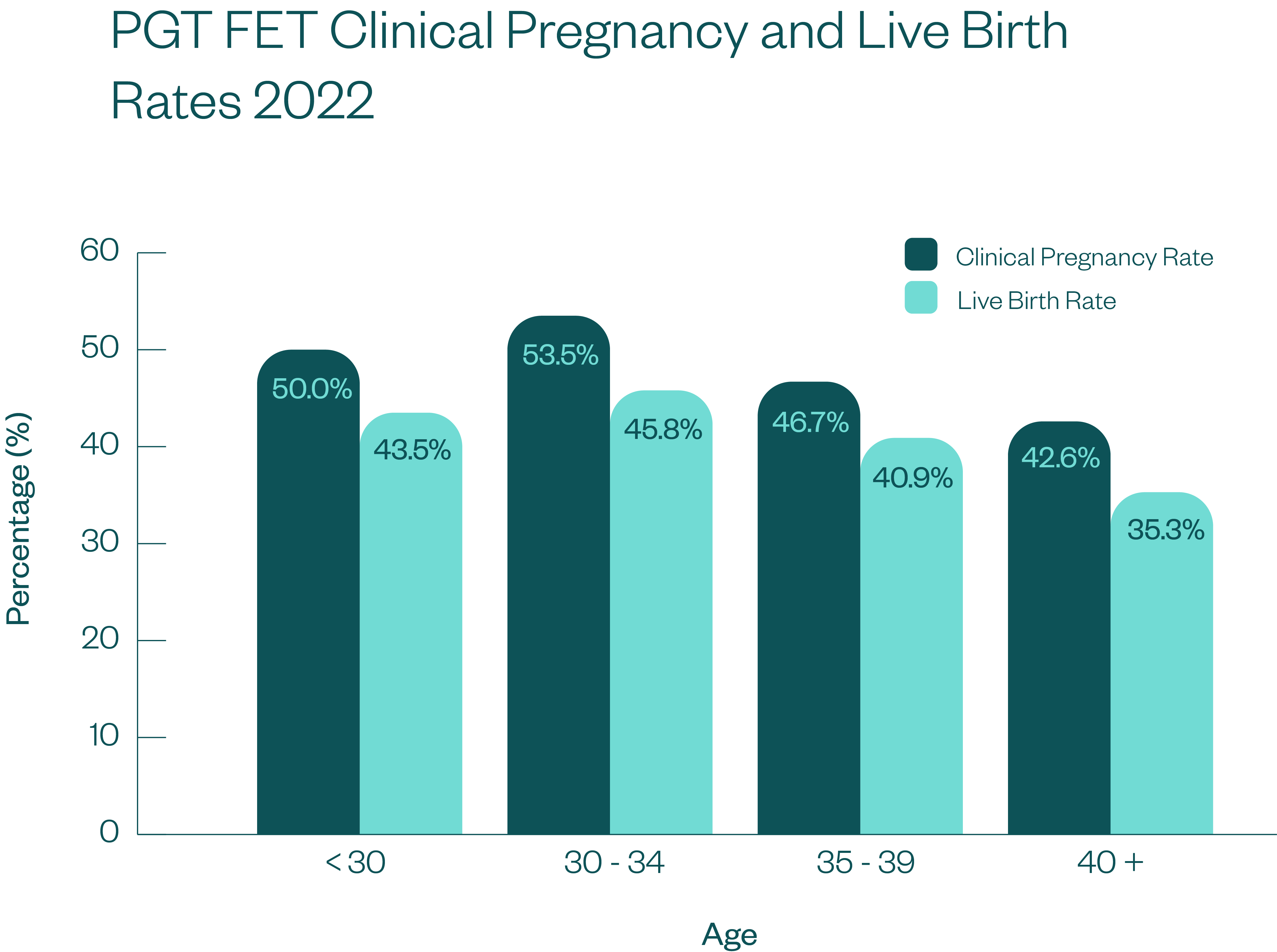
Monash IVF Clinical Pregnancy and Live Birth Success Rates 2022
The clinical pregnancy rates we include below are per the Australian and New Zealand Assisted Reproductive Database (ANZARD) definition. According to ANZARD, a clinical pregnancy must fulfil one of the following criteria:
- known to be ongoing at 20 weeks;
- evidence by ultrasound detection of an intrauterine sac (with or without a fetal heart);
- examination of products of conception reveal chorionic villi; or
- an ectopic pregnancy has been diagnosed by laparoscope or by ultrasound.
Live Birth Definition:
According to the World Health Organisation (WHO) definition, a live birth is defined as the complete expulsion or extraction from its mother of a product of conception irrespective of the duration of the pregnancy, which, after such separation, breathes or shows any other evidence of life, such as beating of the heart, pulsation of the umbilical cord or definite movement of the voluntary muscles, whether or not the umbilical cord has been cut or the placenta is attached; each product of such a birth is considered liveborn.
Our data is not adjusted for:
- Patients with varying lengths of infertility and previous cycle numbers
- Female and male BMI (weight)
- Ovarian reserve parameters
- Male age
- Embryo grade, day of transfer, or survival rates
- Lifestyle factors (e.g. smoking)
- Medication regime used
If you would like to know more about how success rates are interpreted, please see the Fertility Society of Australia's consumer guide here.
Looking to get started with Monash IVF? Contact our friendly nursing team for a complimentary 15-minute chat.
Continuously improving
We are continually striving to improve our success rates and outcomes for our patients. Read about the initiatives we are working on to improve our success rates here.
Your Journey
Many factors can contribute to your likelihood of achieving a pregnancy or live birth. Maternal age is the single most important consideration, but the cause of infertility and lifestyle factors such as weight and smoking also play a part.
We recommend that everyone should have a consultation with a fertility specialist to understand their individual chances of success. A fertility specialist will review your personal medical history, conduct fertility health assessments, and discuss your individual chances of success with you.
It’s important to realise that not every treatment cycle will result in an egg collection, an embryo transfer, or having embryos to freeze. We do everything we possibly can to give you the very best chance of successfully conceiving, but unfortunately, there are no guarantees when it comes to fertility treatment.
Simply put? Your chance of success is very specific to your clinical situation. A fertility specialist can provide you with personalised guidance and fertility advice. You can book a consultation with a fertility specialist here.
Have questions about success rates?
Our team of experienced fertility nurses are available to answer your questions about Monash IVF’s success rates, and provide you with personalised guidance about your fertility. Book a complimentary nurse chat here.

Start your fertility journey
Wherever you are on your journey, one of our supportive nurse enquiry team members can help you understand your options and take the next step. These conversations are free and informative.